Since the official declaration of the Covid-19 pandemic on March 11, there has been much controversy about the use of masks, especially in the first months. However, one aspect has never been questioned: the masks that offer greater protection to the user should be worn by frontline workers of the fight against Covid-19, these men and women who perform essential work in the pandemic and are in daily contact with high concentrations of the Sars-Cov-2 virus in hospitals and cemeteries. Images of doctors, nurses and cemetery workers wearing masks and other PPE (personal protective equipment) have become icons of the pandemic currently affecting the world.
In fact, the masks best suited to protect these professionals are given the technical name of “respirators” (yes, the same term used for devices that help ICU patients to breathe and which have also been protagonists in this pandemic), seeing that their main objective is to filter the air breathed by the user, preventing a large part of the airborne particles (including viral particles) from entering the airways through the nose and mouth.
The respirators recommended for these professionals in the Covid-19 epidemic (certified as N95, KN95, PFF2 or DS2, depending on the country of certification) have high capacity to prevent the passage of particles. But that is not enough. In addition to being good at filtering, respirators need to ensure a minimum of comfort and good airflow so as not to suffocate the user throughout the workday. They also need to be firmly fastened to the head. Finally, they must ensure effective sealing around the mouth and nose to minimize the entry of unfiltered air into the airways of the worker using them. This set of features distinguishes respirators from other types of masks, including surgical masks.

To bring together these characteristics, N95 respirators include a series of developments and advances linked mainly to the materials used and the product design, as well as methods to prove their effectiveness.
Early days: the antiplague mask
The idea of filtering the air to protect people from pathogens that enter the body through the respiratory tract is not new, but it is also not that old. People wearing rigid masks or handkerchiefs to protect themselves from diseases were depicted in Renaissance paintings. However, this protection was associated with several beliefs with no scientific basis, and not with the idea that microorganisms can cause disease, a concept whose discovery dates back to the second half of the 19th century in Europe.
At the end of the 19th century, another step was taken in Europe with the scientific finding that droplets leaving the airways carry bacteria. Consequently, we have the first examples of surgeons using pieces of gauze tied to the head by strings to cover the mouth and nose during surgeries, in order to not contaminate patients.
In 1910, while the use of surgical masks was slowly spreading across Europe, the masks moved on from the operating rooms. More precisely, it was during the so-called “Manchurian plague” – an epidemic that occurred in northern China – that the first clear example of the use of masks is found with the aim of protecting the user, especially doctors, from an infectious disease. In this epidemic, a pathogen (probably a bacterium) caused pneumonia, which, according to the records of the time was lethal in almost all cases. The plague decimated some 60,000 people in less than a year.
It was initially believed that the disease was transmitted by rat fleas, but that idea fell when Dr. Wu Lien-teh was hired by the Chinese government to deal with the epidemic. After performing an autopsy, Wu obtained the necessary evidence to claim that the pathogen was transmitted through the air. Based on this observation, and based on the surgical mask concept he had seen in Europe, he developed a cotton filter mask wrapped in gauze that covered mouth and nose and several layers of cloth wrapped around the head and tied around the neck in order to guarantee that the mask was fastened and sealed the face. Wu called his invention an “antiplague mask” and tried to disseminate its use among those who cared for the sick, and, as far as possible, also among patients and the general population.
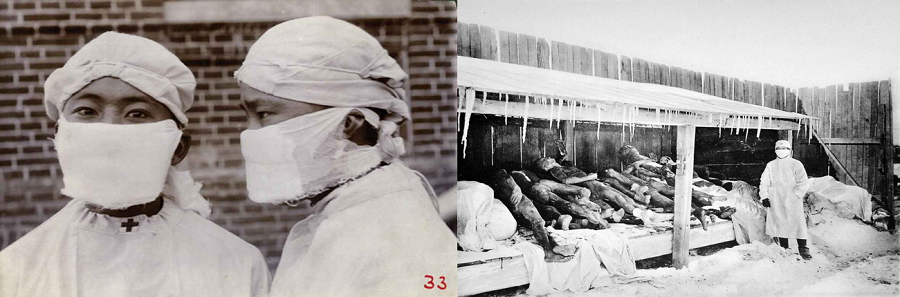
Other mask models appeared at this time in Manchuria, including a hood with eye holes, but Wu’s model seems to have been the one accepted. Apparently, the antiplague mask, with its several layers preventing the passage of droplets and its relatively high filtering capacity, reasonably protected the user from the pathogen. However, some people doubted its effectiveness and also the transmission of the disease through the air. Such was the case with a prominent French doctor who came to Manchuria to work on the epidemic. He denied using the mask, fell ill and died within a few days, according to Wu in his autobiography.
A few years later, in 1918, the use of masks spread throughout the world with the rapid spread of the deadly flu pandemic unjustly called the “Spanish flu”, which was caused by the H1N1 influenza virus and killed 50 to 100 million people in about two years. During this period, the masks, made of gauze and other cotton fabrics, became part of not only the uniforms of doctors and nurses, but also the uniforms of city policemen as well as the soldiers who were still fighting in the trenches at the end of the First World War. These masks were produced more professionally and extensively, with teams of Red Cross nurses cutting and sewing fabrics. In some cities, part of the population adopted this protective accessory, usually made at home. In other cities, its use was mandatory.
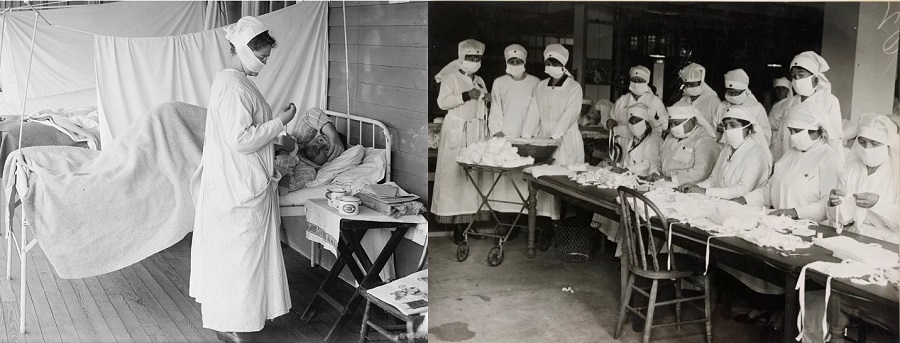
Meanwhile, in the early decades of the twentieth century, doctors were trying to determine which type of mask would be most efficient to protect the user from respiratory droplets carrying microorganisms, and some new models and patents emerged, but without major innovations. These masks were usually made of several layers of cotton gauze. Sometimes they included an additional layer of waterproof material and, in the most advanced models, a metal frame. All these masks were washed or sterilized and reused.
Respiratory protection for industrial workers
At the same time, researchers, companies and governments in countries like the United States were working on the development and regulation of respiratory protection for other workers: those in mining and construction, who were highly exposed to inhaling particles dangerous to their health. This problem was not new. Records from Ancient Rome, in the 1st century AD, show the use of animal skins to cover part of the face in order to filter out the presence of airborne toxic powders. However, in the 1930s, a tragedy forced the need to urgently implement this type of protection. Hundreds of workers died from lung problems caused by inhaling silica dust during the construction of a tunnel in the state of West Virginia, in the United States.
In the late 1950s, in the United States, a woman in her forties propelled the history of the development of respirators. Sara Finkelstein, with a degree in Design, but interested in multidisciplinary approaches, founded the Sara Little Design Consultancy, whose name alluded to her short stature (and her good humor). One of her first works was for 3M, in the company’s wrapping and fabrics division, where a new material for decorative tapes was being tested, the “nonwoven fabric”.
This group of materials is defined and understood through its opposite, the group of fabrics. While fabrics are obtained by weaving or knitting, non-woven fabrics are manufactured using other processes to connect the fibers together. One of the most common processes is meltblowing, in which a molten polymer is blown through a mold with very small orifices by a strong air blast, causing the random deposition of polymeric fibers and thus forming the nonwoven fabric. Another difference: fabrics are ordered structures of threads, usually arranged at right angles; nonwovens, on the other hand, are tangles of crude fibers. With a very porous structure, formed by very small pores and fibers intertwined in a disordered way, nonwoven fabrics are great filtering materials: they let gases pass, while solids are trapped in the fiber maze.
But back to Sara Little: aware of the impact materials innovation can generate not only in a company, but also in the lives of consumers of the final products, she made a presentation to 3M directors proposing the many possibilities for the application of nonwoven materials, recommending the development of a business area dedicated to these materials. At that time, the nonwoven industry was very new in the United States, as well as in Europe; it is estimated that the production of these materials on a pilot scale started in the 1930s.
Apparently, Sara Little designed, for 3M, some products using nonwoven fabric, starting with a bra cup. The idea and design of the first 3M respirator, with its semicircular shape resembling a bra, the clip to seal the mask over the nose and the elastics to fasten it to the head is mainly attributed to her. It is said that Sara’s intention was to create protection for hospital workers, whose routine she had known personally after many years of accompanying sick family members. However, at that moment there was no consensus regarding the health professionals’ need to use respirators, except for the use of masks during surgical procedures, which were mainly aimed at protecting patients from the doctors’ respiratory secretions and protecting doctors from blood and other patient fluids.
At 3M, the first respirator was launched in the early 1960s, with no official certification but with proof of its efficiency in filtering powders, which is so necessary to protect workers exposed to inhaling harmful particles in mining, construction and car painting activities, among others. In 1972, 3M was the first company to introduce a certified respirator to the market.
Respirators for doctors and nurses
Regarding the filtration of microorganisms, at that time there was no clear evidence, but some records show that these respirators, manufactured on an industrial scale, were sold to doctors and nurses who wanted to protect themselves. With the introduction of nonwoven materials replacing fabrics, disposable masks began to enter hospitals, a well received novelty at the time as it reduced costs related to washing and sterilization personnel and, at the same time, brought more sanitary security.
For about twenty years, with no major news of diseases transmitted by respiratory droplets or airborne, N95 respirators have spread and were recognized as respiratory protection equipment in the industry. However, in the 1990s, the use of this personal protective equipment increased in hospitals given the outbreaks of antibiotic-resistant tuberculosis that had infected many health professionals.
In the same decade, new technologies absorbed by the industry allowed to further improve the performance of respirators, especially with regard to the retention of smaller particles, such as viruses. With these processes, which have some patents, it was possible to generate an electrostatic charge in the fibers of the nonwoven material, which attracted the particles – somewhat similar to what happens when pieces of paper stick to a balloon that has been rubbed against a wool coat. Thanks to this strategy, the capacity of respirators to retain particles has increased without having to add new layers of filtering material, thus preserving the good air intake that respirators must provide.
One of the researchers involved in patents on processes for electrostatic charge of nonwoven materials has gained a lot of visibility recently. This is Peter Tsai, who made his contributions while professor at The University of Tennessee, in the United States. Tsai returned to scientific activity in March of this year shortly after retiring. As a specialist in the manufacturing and treatment processes of the nonwoven materials used in masks, Tsai has been working to help establish safe sterilization mechanisms for N95 respirators, given the scarcity of this product generated by the Covid-19 pandemic.
With all these advances in materials, technologies, concepts and methods, respirators have entered the 21st century ready to help healthcare workers reduce the risk of infection from viral diseases that are transmitted through droplets and respiratory secretions, and even through the air. And they really helped. N95 respirators were recommended for health personnel in the 2002 and 2003 SARS epidemic, in the Mers outbreaks that have been occurring since 2012, in the 2009 swine flu pandemic and, currently, in the Covid-19 pandemic.

To learn more:
- https://www.fastcompany.com/90479846/the-untold-origin-story-of-the-n95-mask
- https://en.wikipedia.org/wiki/Wu_Lien-teh
- https://www.tandfonline.com/doi/full/10.1080/01459740.2017.1423072
- https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(20)31207-1/fulltext
- https://www.nytimes.com/2020/02/13/opinion/coronavirus-face-mask-effective.html
- https://www.textileworld.com/textile-world/nonwovens-technical-textiles/2012/05/introduction-to-nonwovens-technology/
- https://designmuseumfoundation.org/ask-why/
- https://www.cdc.gov/niosh/npptl/Respiratory-Protection-history.html
- https://utrf.tennessee.edu/ut-researchers-nonwoven-fabrics-protect-the-health-of-more-than-a-billion-people/
